This abstract was presented today, May 2th at the 2016 Association for Research in Vision and Opthalmology (ARVO) meetings in Seattle, Washington by Jefferson R. Brown, Rebecca L. Pfeiffer, Crystal Sigulinsky, Felix Vazquez-Chona, Daniel Emrich, Bryan W. Jones, Robert E. Marc.
Abstract Number: 995
Author Block: Jefferson R. Brown1 , Rebecca L. Pfeiffer1 , Crystal Sigulinsky1 , Felix Vazquez-Chona1 , Daniel Emrich1 , Bryan W. Jones1 , Robert E. Marc1
1 Dept of Ophthalmology, University of Utah, Salt Lake City, Utah, United States
Disclosure Block:Jefferson R. Brown, None; Rebecca L. Pfeiffer, None; Crystal Sigulinsky, None; Felix Vazquez-Chona, None; Daniel Emrich, None; Bryan W. Jones, None; Robert E. Marc, Signature Immunologics (Code I (Personal Financial Interest) )
Purpose:Retinal vasculature is strongly affected by degenerative pathologies and in turn, may also contribute to their progression. However, much of what we understand about the normal, healthy interaction between neurons, glia, and blood vessels at the ultrastructural level is limited to single section electron microscopy. The technology of serial section transmission electron microscopy (ssTEM) extends the high definition of TEM imaging into three dimensions to create volumes, allowing for more thorough visualization and analysis of the vascular-glial-neuronal complex.
Methods:RC2 is a 40TB ssTEM volume of over 1,400 horizontal sections of retinal tissue derived from an adult female C57BL/6J mouse. The tissue sample is 250 um in diameter and spans the outer nuclear layer to the vitreal surface. Baseline resolution is 2.18nm per pixel. Visualization, navigation and metadata annotations of the database are made via the Viking software suite.
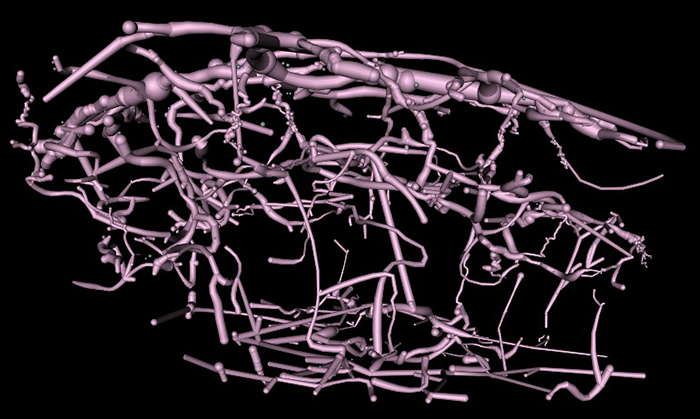
Results:Much of the retinal vascular basement membrane directly contacts Muller cells. In the ganglion cell layer, direct basement membrane contact with astrocytes is frequent. Microglia commonly contact the basement membrane, and occasionally direct contact of neurons onto basement membrane was observed. Full 3D reconstruction of all vascular pathways with associated endothelia and pericytes within the volume was completed, demonstrating that all the retinal capillary layers are continuous with one another [Figure].
Conclusions:The presence of occasional direct neuronal contact onto vascular basement membrane supports earlier work by Ochs and colleagues (2000) and suggests the blood-retina barrier does not universally involve retinal glia. However, since such contacts are extremely sparse, it remains to be seen whether this finding has biologic significance, though their existence suggests significance. The RC2 volume is a valuable resource to aid in discovery of defining characteristics of wild type neurovascular architecture.
The intro figure is a side view of reconstruction of all vasculature within the RC2 volume. Vessels at the top of the figure correspond to the outer plexiform layer, while those at the bottom correspond to the ganglion cell layer. This capillary plexus is one continuous structure. Visualization by VikingView software.